
By Dr. Pascal Sacré
Global Research, November 01, 2020
Introduction
 COVID-19 appeared in Europe and the Americas in 2020, following the emergence of a new virus from China in 2019. This new virus belongs to the well-known family of coronaviruses that has already produced two particularly severe epidemics in 2003 and 2012.
COVID-19 appeared in Europe and the Americas in 2020, following the emergence of a new virus from China in 2019. This new virus belongs to the well-known family of coronaviruses that has already produced two particularly severe epidemics in 2003 and 2012.
This new virus is called SARS-CoV-2, the third coronavirus responsible for a severe respiratory distress syndrome.
The severity of this syndrome is mainly characterized by hypoxemia, a lack of oxygen in the blood.
We have found that this severe lung involvement is seen in a relatively small number of patients infected with SARS-CoV-2, most of whom are asymptomatic or have only an influenza-like illness or even a common cold.
For the most severely affected patients, mainly elderly people and/or people weakened by one or more chronic diseases (heart, respiratory and kidney failure, diabetes, high blood pressure, obesity, etc.), mortality would be slightly higher than for seasonal influenza, the precise figures still need to be evaluated.
These figures are still controversial today, with some scientists and physicians arguing, with supporting evidence, that mortality has been overestimated by official health centers.
I felt it was important to clarify several points in relation to this coronavirus, SARS-CoV-2, with COVID-19 disease, with its clinical and radiological diagnosis, and especially with the RT-PCR technique used as the main screening tool.
I conclude with a few words on the mode of transmission of the virus, by aerosols and airborne particles, implying in particular the importance of properly ventilating confined spaces.
1. Virus Size
1 millimeter (mm) = 1000 micrometers or microns (μm) = 1,000,000 nanometers (nm)
Diameter of a human hair: 150 micrometers (μm)
Size of SARS-CoV-2 coronavirus: 0.125 μm (125 nm), 1/1200th of hair
Influenza virus (Influenzavirus) size: 0.08-0.120 μm (80-120 nm)
2. The Coronavirus2 and COVID-19
Coronavirus or CoV = RNA virus (ribonucleic acid)
1. DNA and RNA
DNA or deoxyribonucleic acid
Deoxyribonucleic acid or DNA is a biological macromolecule present in all cells as well as in many viruses. DNA contains all the genetic information, called the genome, that allows the development, functioning and reproduction of living beings.
The genome is made up of genes composed of DNA or RNA.
Let’s symbolize the DNA double helix by a ladder :
DNA is formed of two strands RNA is formed of paired pairs of one of the two strands.
All cells contain DNA or RNA, even viruses that are not cells but particles, genetic material (DNA or RNA) surrounded by a capsule or nucleocapsid.
Such particles cannot be said to be “alive”, they are packets of information gathered on a gene carrier (genes forming a genome).
Viral particles use the cells they infect (parasitize) to replicate (reproduce) their genome (DNA or RNA) and multiply.
In doing so, they kill the host cell and trigger a defensive response from the invaded organism.
Coronavirus CoVs are RNA viruses, such as Ebola, Zika, measles, influenza.
CoVs are the largest RNA viruses.
The herpes virus (chickenpox) is a DNA virus.
Corona Viruses or CoVs
They form a huge family of viruses.
Their genome (RNA) is very long: several thousand (30,000) nucleotides or bases forming a single-stranded linear RNA coding for 7 to 10 proteins.
They are surrounded by a crown-shaped protein capsule.
Humans can be infected by 5 major types of coronavirus :
- HCoV-229E, HCoV-OC43 causing common colds and benign flu-like symptoms.
- SARS-CoV-1 responsible between November 2002 and July 2003 for an epidemic of severe acute respiratory syndrome (SARS).
- MERS-CoV responsible for an epidemic of severe respiratory syndrome in 2012, mainly in the Arabian Peninsula (starting in Saudi Arabia) but also in South Korea. MERS for Middle-East Respiratory Syndrome.
- SARS-CoV-2, very similar to SARS-CoV-1, responsible for an epidemic of severe respiratory syndrome that has evolved into a pandemic. Beginning in 2019. The disease caused by SARS-CoV-2 is called COVID-19 for COrona VIrus Disease, which appeared in 2019.
So, let’s remember that the most frequent coronaviruses in humans are commonplace and responsible for 30% of annual colds, along with other viruses, especially rhinoviruses.
Let’s also remember that coronaviruses, like many viruses, have an important capacity for evolution and adaptation (mutation), which can lead to the appearance of variants and more or less pathogenic viruses.
3. SARS-CoV-1: Severe Acute Respiratory Syndrome-CoV-1
First known coronavirus to cause serious disease in humans.
Epidemic between November 2002 and July 2003.
More than 8,000 cases in 30 countries (20% of cases in caregivers).
774 deaths or about 10% mortality.
Moderate transmissibility (contagiousness).
Exceptional capacity for mutation and recombination.
Complete sequencing of the SARS-CoV-1 genome by American and Canadian research teams.
4. MERS-CoV: Middle-East Respiratory Syndrome-CoV
The second coronavirus known to have caused severe disease in humans.
First cases in 2012, in Saudi Arabia.
More than 1500 cases, in 26 countries, mostly in the Arabian Peninsula and South Korea.
More than 550 deaths, a very high mortality rate of 30%.
5. SARS-CoV-2: Severe Acute Respiratory Syndrome-CoV-2
Third coronavirus known to have caused serious disease in humans, a disease called COVID-19 for Corona VIrus Disease, 19 for the year it began, 2019.
The mortality due to SARS-CoV-2 (COVID-19), known as of 29-09-20 and specified on the Worldometers site, would be 1 million deaths.
https://www.worldometers.info/coronavirus/?
SARS-CoV-2 is believed to have emerged in China in late spring/early summer 2019 and in Europe in October 2019.
[Links: https://hal.archives-ouvertes.fr/hal-02930784
https://hal.archives-ouvertes.fr/hal-02886806 ]
Its genetic sequencing is updated (following frequent mutations) on the website :
It is also closely monitored by the laboratory of Professor Didier Raoult’s team in Marseilles at the IHU-Méditerranée.
[Link : https://www.youtube.com/watch?v=Lvb7OSAKbfo ]
6. Vaccine
NO vaccine to date against SARS-CoV (2003) or MERS-CoV (2012)!
Yet in COVID-19, the whole world is waiting for a vaccine, counting on one vaccine if possible in a few months!
Between 1999 and 2017, the world’s 11 largest laboratories made €1019 billion in profits, of which €925 billion (90.7%) was distributed to their shareholders. 925 billion (90.7%) was distributed to their shareholders.
Here, the vaccine industry, which is relatively modest (3% of global sales in 2009), presents itself, with the rise of biotechnology, as the most dynamic niche (growth of 24% between 2011 and 2014).
This branch of the pharmaceutical industry is dominated by four groups (Merck, Sanofi, GSK and Pfizer) accounting for 65% of sales.
Groups from developing countries are asserting themselves on the remaining market shares: Serum Institute and Biological E (India), Butatan Institute and Bio-Manguinos (Brazil), CNBG (China)… Today, specialists [who have endorsed the official narrative] seem to be unanimous in affirming that the main challenge is the development of a vaccine against Covid-19.
7. Clinical picture
A. Incubation period (time between infection and onset of symptoms) :
SARS-CoV-1 and SARS-CoV-2: 2 to 7 days
MERS-CoV: 5 to 15 days
It is on the first day of symptoms that the individual is most infectious (highest viral load and high capacity to project it by coughing). He must be isolated!
In the acute epidemic phase (March-April 2020) excretion of 700,000 copies of viral RNA/μl on the first day of symptoms. Excretion of 700,000,000 copies of viral RNA/μl after a few days of symptoms!
B. Diagnosis is primarily clinical (symptoms) :
a. Major symptoms :
- Cough
- Dyspnea (difficulty breathing) with desaturation of blood oxygen (O2)
- Chest pain
- Anosmia (loss of sense of smell)
- Dysgeusia (taste disorder) with no other apparent cause
b. Minor Symptoms :
- Fever
- Fatigue
- Rhinitis or colds (runny nose)
- Sore throat (angina)
- Headache (headache)
- Anorexia (loss of appetite) – slimming
- Aqueous diarrhea (liquid stool) with no other apparent cause
- Acute confusion (orientation disorder)
- Sudden falls with no other apparent cause
Note that a loss of smell and abnormal taste can be due to a deficiency in zinc, a trace element or trace that plays an important role in our immune defenses!
Signs suggestive of zinc deficiency :
– Agueusia or dysgeusia, taste disorder. Zinc intervenes in the synthesis of gustin, an essential protein for the perception of taste in taste buds.
– An anosmia, loss of sense of smell.
These signs, would be, according to certain studies, the 1st signs of an infection by the coronavirus. It is therefore highly probable that over-solicitation of the immune system leads to an increase in zinc deficiency, causing these symptoms in some subjects.
[Links: https://www.ncbi.nlm.nih.gov/pubmed/25715353 &
Hiroyuki YANAGISAWA, Zinc Deficiency and Clinical Practice JMAJ 47(8): 359-364, 2004].
Clinical score.
If the score is >/= 2, COVID-19 is suspected. You can see it, you get there quickly and these symptoms are not specific!
Strategy to categorize the severity of the condition and to best guide each person according to their condition and/or its possible evolution.
EWS score for Early Warning Signs :
The severe form (admission to intensive care, with risk of death) of COVID-19 strikes people who are weak, immunocompromised and/or suffering from severe chronic pathologies such as diabetes, kidney failure, chronic lung disease, heart disease, obesity.
Severe risk factors:
BMI = Body Mass Index = Weight divided by height2
Example: Weight 100kg height 1.70m ➔ BMI = 100/1.72 = 34 Severe obesity
C. Chest CT-scanner
This test provides an imaging of the lungs to confirm the diagnosis of COVID-19, for example in case of negative RT-PCR despite a positive clinical picture (Clinical Score >/= 2).
Normal lung CT-scanner :
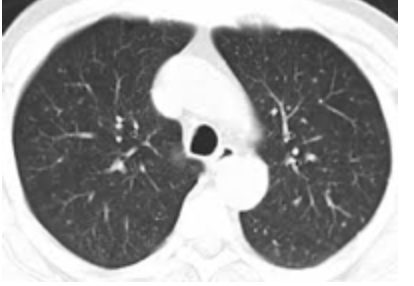
Abnormal lung CT-scan: Rx Thorax:

WARNING, these images are not specific to a COVID-19!
They are found in a group of pulmonary pathologies grouped under the generic term ARDS (Acute Respiratory Distress Syndrome) or SDRA (Syndrome de Détresse Respiratoire Acute).
https://fr.wikipedia.org/wiki/Syndrome_de_d%C3%A9tresse_respiratoire_aigu%C3%AB#:~:text=The ARDS%20Definition%20task%20force,des%20notions%20d’acute%20lung]
ARDS or ARDS can be caused by a large number of causes, intra- or extra-pulmonary, infectious or non-infectious.
Intrapulmonary causes :
- Bacterial, viral pneumonia (influenza, respiratory syncitial virus or RSV, SARS)
- Chemical pneumopathy (inhalation of digestive fluid) or smoke inhalation
- Thoracic trauma
Extra-pulmonary causes :
- Pancreatitis (generalized inflammation of the pancreas with necrosis)
- Extra-pulmonary infections with severe sepsis (infection) and/or septic shock
- Extensive burns
- Cardiogenic shock (heart failure of any origin)
Etc.
So, as we can see, frosted glass lesions are typical of ARDS (or ARDS), not of any particular cause.
They are found in particular in infectious pneumonia with so-called atypical germs, such as Mycoplasma Pneumoniae, Chlamydia Pneumoniae or Legionella Pneumophila, but also in non-infectious pneumopathies.
A differential diagnosis must always be made, especially in people with one or more severe co-morbidities (diabetes, obesity, chronic kidney, lung or heart disease, etc.), which is the case for most people admitted to intensive care units during the COVID period.
The problem is to withhold a diagnosis of COVID without considering other possible causes, especially in the case of a negative RT-PCR.
ARDS has been a common condition since its discovery in 1967 (Ashbaugh DG, Bigelow DB, Petty TL, Levine BE, “Acute respiratory distress in adults”, The Lancet, 1967;2:319-323).
It accounts for about 10% of ICU admissions, with a mortality rate of 40-50%.
[Link: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5537110/ ]
However, all intensive care units in the world consider a positive COVID diagnosis in case of respiratory symptoms (score >/= 2) and a pulmonary CT-scan of ARDS (ARDS), even if the PCR is negative and despite the lack of specificity of the symptoms and the CT-scan.
In this Swiss article published in 2020 in the Swiss Medical Journal (RMS), physicians insist on the limits of the pulmonary CT-scanner for the diagnosis of COVID19 :
“... its specificity is limited, exposing it to the risk of over-diagnosis. »
D. PCR or Polymerase Chain Reaction
The oropharyngeal or nasopharyngeal smear with PCR analysis is the first diagnostic test proposed to confirm infection with COVID-19 SARS-CoV-2.
Molecular biology technique OR gene amplification technique (deoxyribonucleic acid-DNA or ribonucleic acid-RNA genes see pages 2 & 3).
PCR was developed in the 1980s by Kary Mullis, a chemist who won the Nobel Prize in Chemistry in 1993.
“… these PCR tests cannot detect any virus”.
He really said that (https://www.weblyf.com/2020/05/coronavirus-the-truth-about-pcr-test-kit-from-the-inventor-and-other-experts/)
Since 1992, the technique can be carried out continuously, in real time, hence its modern name :
RT-PCR: Real Time-Polymerase Chain Reaction or Real Time Polymerase Chain Reaction
This technique makes it possible to highlight traces of something invisible to the naked eye or even under the microscope.
It is mainly used in industry or criminology to search for traces of DNA.
In medicine, its field of application, in addition to research, particularly in genetics, is infectiology, which studies infectious diseases.
In particular, PCR can reveal germs or microorganisms that are difficult to cultivate, such as certain bacteria (Mycoplasma, Chlamydiae, Mycobacterium Tuberculosis) and viruses.
It is the reference technique for looking for traces of respiratory viruses (influenza, SARS).
PCR does not reveal viruses, but genetic sequences (bits) of the virus, which allows the presence of the virus to be deduced.
This notion is important.
Diagnosis by PCR is an inference that can be subject to misinterpretation.
SARS-CoV-2 is an RNA virus with 30,000 base pairs (bp). Its entire genome should not be highlighted, but only specific sequences.
The SARS-CoV-2 genome is known (see page 5).
Laboratories use SARS-CoV-2-specific gene primers.
To make a reliable PCR result, at least 2-3 genes must be used as primers.
3 genes is best and the technique must be done for all 3 genes.
How does it work?
i. Sampling of cells from the person’s airways.
Sampling just from the throat, nose or saliva shows a lower detection sensitivity (higher risk of false negative).
The first source of error, a false negative, comes from there, a poorly performed sample.
This collection of cells from the back of the pharynx, approached through the nose or mouth, must be performed by a specialized and trained caregiver. It is NOT ANODINOUS! This sample may cause bleeding, damage the pharyngeal (surface) mucous membrane, and/or the nasal mucous membrane if approached through the nose.
ii. Analysis by RT-PCR4
This machine works like a photocopier/enlarger.
The technique has the best sensitivity (90%) and specificity (100%), better than all other conventional tests for pathogen detection (antigenic tests, virus culture). Saliva samples do not meet the required requirements.
Link: To KK &al. Temporal profiles of viral load in posterior oropharyngeal saliva samples and serum antibody responses during infection by SARS-CoV-2: an observational cohort study. Lancet Infect Dis. 2020 May ;20(5) :565-574].
It uses several amplification (magnification) cycles while multiplying the target by 2 on each cycle.
1st cycle: target x 2
2nd cycle: target x 4
3rd cycle: target x 8
4th cycle: target x 16
5th cycle: target x 32
Etc.
Up to 30 to 40 cycles.
Ct or Cycle Time or Cycle Threshold defines the threshold of cycles at which the laboratory considers the PCR assay positive.
The lower the Ct threshold used, the higher the viral load (the more virus in the subject’s respiratory tract).
The higher the Ct threshold used, the lower the viral load (less virus in the respiratory tract).
The RT-PCR is a very sensitive test and by increasing the Ct (up to 40, 50), we can find genetic traces of the virus while it does not correspond any more to a state of infection or contagion!
Knowing the threshold Ct used by the laboratory is thus essential to correctly interpret an RT-PCR result!
Currently, RT-PCR only gives a qualitative result: positive or negative.
It is necessary to give a quantitative result which alone reflects the real importance of the viral load.
At the heart of the acute epidemic phase (March-April 2020), on the first day of symptoms (coughing), the individual was able to excrete up to 108 (100,000,000) copies of SARS-CoV-2/μl viral RNA for a period of 5 days to 5 weeks, with no correlation between the quantity of viral segments detected or the duration of this detection, and the severity of the disease.
Today (September 2020), with a threshold Ct of 32 cycles, 10 to 15 copies of SARS-CoV-2/μl viral RNA are detected, i.e. much less.
With a threshold Ct of 35 cycles (standard threshold Ct for laboratories in France and for the European CDC), this corresponds to 1 copy of SARS-CoV-2/μl viral RNA sample!
[Links : Bullard J. et al, 2020, https://covidaba.com/wp-content/uploads/2020/05/Predicting-infectious-SARS-CoV-2-from-diagnostic-samples.pdf
ECDC gives a threshold of 35 https://www.ecdc.europa.eu/en/all-topics-z/coronavirus/threats-and-outbreaks/covid-19/laboratory-support/questions ]
Above the Ct threshold of 35, it is impossible to isolate a complete viral sequence.
(Data transmitted by Hélène Banoun, https://www.researchgate.net/profile/Helene_Banoun
PhD, Pharmacist biologist. Former INSERM Research Fellow. Former intern at the Paris Hospitals and shared by the French biologist Pierre Sonigo, specialist in molecular biology and virology, https://fr.wikipedia.org/wiki/Pierre_Sonigo.)
The correct interpretation of RT-PCR depends on :
- The knowledge of the threshold Ct or copy number of viral RNA/μl, reflecting the viral load
- The clinical condition of the person being tested
1 copy of viral RNA/μl is equivalent to 1000 copies of viral RNA/ml collection. Please pay attention to the unit returned by the laboratory!
The first point gives an indication of the degree of contagiousness.
The second point gives an indication of the degree of severity.
An RT-PCR test alone, positive, means absolutely nothing, especially outside of epidemic periods, such as today (September 2020) as evidenced by the reasonable level of hospital admissions, intensive care and deaths.
Basing medicine on a single test, without correlating it to the clinic, exposes to the risk of SURDIAGNOSIS.
Asking asymptomatic people to line up in front of laboratories to do an RT-PCR test, or letting people do it, makes no sense other than to impose an unnecessary cost to society, to maintain the fear of an absent disease since the people in these queues are asymptomatic and tip the benefit/risk balance dangerously in their favour.
It would be like asking everyone to have an electrocardiogram, even in the absence of any symptoms!
Physicians should require knowledge of the threshold Ct used to define a positive PCR test (or the number of copies of viral RNA/μl sample) in order to correctly interpret the result.
All laboratories should use the same standardised standards, the same cut-off Ct, if possible a cut-off Ct </= 30 and express the result as the number of copies of viral RNA/μl sample.
III. VIRUS: DIFFUSION IN THE ATMOSPHERE and the value of ventilating any space5
Respiratory viruses are not transmitted individually (virion), but in groups in the form of larger particles:
1. Particles G = microdroplets that form an aerosol: 5 to 150 μm
Transmission through coughing, sneezing or talking from an infected person
Dense and rich in water, heavy, they remain in the air for a short time and are only diffused over short distances: < 1 m, then fall to the ground quickly.
[Link : https://www.thelancet.com/journals/lanres/article/PIIS2213-2600(20)30245-9/fulltext ]
2. Particles A = Airborne particles: < 5 μm
Low density and low water content, A particles are lighter, remain suspended in the air and have a greater range.
[Links: https://www.nejm.org/doi/pdf/10.1056/NEJMc2004973?articleTools=true ]
Summary
SARS-CoV-2 is a 125 nm RNA virus (0.125 μm), with +/- 30,000 base pairs (nucleotides).
It causes the disease COVID-19 (COronaVIrusDisease-2019).
It is projected by G particles (aerosols > 5 μm) heavy over < 1m and by A particles (< 5 μm) light over long distances: interest to ventilate closed spaces!
The diagnosis is above all clinical:
- Symptoms forming a clinical score, suspicion of COVID-19 if clinical score >/= 2
- Evaluation of the severity of COVID-19 by the Early Warning Score: EWS (Early Warning Signs)
- Symptoms are not very specific and can be found in any viral (flu, cold, SARS) or even bacterial disease.
Diagnosis completed by a lung CT-scan: image of ARDS (or ARDS-acute respiratory distress syndrome): the CT-scan image is not specific for COVID-19!
Diagnosis by RT-PCR technique for Real Time-Polymerase Chain Reaction: qualitative examination expressed by the positive or negative sign.
- False negatives exist from the sampling to the last amplification by PCR, because the technique is complex and subject to potential handling errors. There are few or no false positives (high specificity).
- RT-PCR reveals pieces (gene sequences) of the SARS-CoV-2 virus, not the virus itself, and this search is done using primers, i.e. 2 or (better) 3 known SARS-CoV-2 genes.
- The quantitative aspect (viral load) is given by the number of amplification cycles (Ct for Cycle Time or Cycle Threshold) used as a positivity threshold. The lower the threshold (Ct), the higher the viral load, the more virus, the sicker and/or more contagious the person is. The higher the threshold (Ct), the lower the viral load, the less virus there is, the less sick and/or contagious the person is.
- In the current period (September-October 2020), there is no interest in performing RT-PCR in asymptomatic people!
- Today, the thresholds of positivity (Ct) of RT-PCR are too high (>/= 35), inducing an “epidemic” of positive tests that do not mean anything anymore (false positives), neither epidemiologically nor in terms of public health!
- Positive thresholds (CT) for RT-PCR should be standardized for all laboratories, reported in the results and should be below 35 (even 30).
Pulmonary CT-scan and RT-PCR with a positivity threshold (Ct) >/= 35 induce a dangerous OVERDIAGNOSIS when the subject is not evaluated to see if he is sick first, which is the only thing that really matters.
“To interpret the result of a PCR, it is essential that clinicians and microbiologists share their experiences so that the analytical and clinical levels of interpretation can be combined” PCR in Microbiology, RMS, 2007
Dr. Pascal Sacré is a physician specialized in critical care, author and renowned public health analyst. He is a Research Associate of the Centre for Research on Globalization
Translation from French by Global Research



























